Pediatric Mental Health Training for Residency Programs
Resident Education in Anxiety, Depression and Suicidality (READS) gives residency faculty the skills, confidence, and turnkey tools to teach evidence-based assessment and treatment of anxiety, depression, and suicidality to their residents.
Join the Notification ListWHO IT’S FOR
Designed for the Faculty Shaping Residency Mental Health Training
READS is built for pediatric residency core faculty, child and adolescent psychiatrists, psychologists, and any clinician responsible for resident mental health education. If you shape how the next generation of clinicians learns to care for children’s mental health, READS is for you.
Most pediatric residents graduate without adequate training in mental health. READS changes that by equipping residency faculty with the skills, confidence, and ready-to-use teaching materials to deliver high-quality mental health education to their residents.
This faculty development program focuses on evidence-based assessment, diagnosis, and treatment of anxiety, depression, and suicidality in children and adolescents. Faculty leave not just better trained themselves, but prepared to teach.
The program includes three components:
10 hours of live, expert-led training
delivered virtually across two focused half-day sessions.
A complete, turnkey teaching
toolkit
everything faculty need to begin teaching immediately, including:
- PowerPoint slides for use with residents
- Video recordings of READS training sessions
- Public domain rating scales for anxiety, depression, and suicide risk
- Handouts for residents — diagnosis, treatment, and clinical algorithms
- Dosing guides and medication cards
- Handouts for families and caregivers
Four follow-up implementation sessions
live group calls after the training to help faculty:
- Support implementation with their residents
- Troubleshoot teaching challenges
- Deepen clinical knowledge
- Prepare to confidently answer resident questions
Course dates
Join the notification list to be alerted as soon as new dates are available.
Join the Notification ListHear from READS participants
Hear from the educators who have completed READS and brought transformative mental health training into their residency programs.
“Bringing together a group of motivated academic pediatricians to discuss the importance of teaching behavioral health to residents is such a gift from REACH. We need to tackle this issue as a team and share resources and strategies.”
— Catherine Kent, MD
Pediatrician, Portland, OR
Having the ongoing training and being able to talk to your peers AND have some support from instructors really did help with confidence building. You always question yourself and whether you’re doing the right thing… but when you see improvement, especially working with families and children, it reaffirms that you’re on the right track.
Kristin Mason, LCMHC, MSW, ESMHL
Vermont
Participants earn up to 13.75 CME credits
CME Accreditation
In support of improving patient care, the University of Arkansas for Medical Sciences and The REACH Institute are jointly accredited by the ACCME, ACPE, and ANCC to provide continuing education for the healthcare team.
AMA Credit Designation
This live activity is designated for a maximum of 13.75 AMA PRA Category 1 Credits™. Physicians should claim credit commensurate with their participation.
READS Questions Answered
Everything residency faculty and program directors need to know
about READS — how it works, who it’s for, and how to get started.
The Parent Empowerment Program (PEP) is a REACH training designed for family peer advocates — parents and caregivers of children with mental health challenges who support other families in similar situations. PEP equips participants with clinical knowledge, advocacy skills, and practical tools to help families get the care their children need and deserve.
PEP is for parents and caregivers of children with mental health conditions who work in a peer advocate role — supporting other families navigating diagnosis, treatment, and systems like healthcare and schools. PEP is typically organized by healthcare systems, school districts, or community organizations that want to strengthen family advocacy in their community.
PEP covers the critical knowledge and skills peer advocates need — including problem-identification and priority-setting, engagement, listening and boundary-setting, group management, mental health evaluation, diagnosis and treatment, the mental healthcare system, and school systems and special education options. Participants also receive a comprehensive family empowerment manual and ready-to-use materials.
PEP consists of two components: a five-day interactive seminar, followed by 12 follow-up consultation calls held twice a week over six months. The full program is designed to build knowledge during the seminar and reinforce implementation through sustained consultation support over time.
PEP is delivered to groups of 15 or more and is organized through REACH’s group training infrastructure. Healthcare systems, school systems, and community organizations can schedule and host a PEP training for their community. Contact REACH’s group training team to discuss scheduling and delivery format.
Yes. REACH offers specialized PEP programs tailored for child welfare and juvenile justice settings — designed to help parents and staff work together to address the mental health needs of children involved in those systems. Specialized tracks are available as part of group training arrangements and can be customized to your organization’s needs.
All PEP participants receive a high-quality family empowerment manual and supporting materials — practical, ready-to-use resources that help peer advocates apply their learning and support other families with confidence.
Visit REACH’s Group Training page to learn more about scheduling a PEP for your group. PEP is available for groups of 15 or more and can be organized by healthcare systems, schools, and community organizations. Our team will work with you to find the right format and timeline.
Yes. Join the PEP waitlist to be notified when new training dates or group opportunities become available. You can sign up directly on this page.
Still Have Questions?
Our team is ready to help you find the right training solution for your organization and those you serve.
CONTACT USAdditional Resources
Class aptent taciti sociosqu ad litora torquent per conubia nostra, per inceptos himenaeos. Duis vehicula, libero vitae malesuada elementum, lectus lectus vestibulum neque, sed pretium nunc justo in metus.

Helping patients through divorce
“Parents who are going through a divorce really want to believe their children are OK,” said Lisa Blum, PsyD, a licensed clinical therapist on the faculty of The REACH Institute’s CATIE program. “They’re terrified that they’re hurting their kids. So if Sally is doing her homework and Johnny isn’t acting out, the parents think, ‘Whew, good, they’re fine!’ But often they’re not fine.” Though divorce rates in the US have been declining for years – including, according to early reports, during 2020 – the rates are still high. Each divorce or separation brings loss, disruption, and pain to any children involved.

New coding guidelines for 2021
2021 brings big changes to coding for mental health visits in pediatric primary care! The new coding guidelines issued by the Centers for Medicare and Medicaid Services (CMS) reduce the documentation burden and increase the levels of payment (work relative value units or wRVUs).

10 ways to help families through the holidays
If you’re like most pediatric primary care providers (PCPs), you’ve seen an increase in child mental health issues due to COVID. Research shows that the pandemic, with its consequent disruption and isolation, has increased adolescents’ risk of trauma, depression, and anxiety. Families are dealing with grief, the anxiety of whatever “school” means this week or this month, and, in many cases, loss of income. Families of color and low-income families have been hardest hit by the pandemic itself, by the economic and social fallout, and by the attendant impairment of mental health. And now come the holidays.

Working with challenging families
You’re in the consultation room with Anita, who first brought her 15-year-old son Vic to you two weeks ago. Vic has been suspended from school several times for increasingly dangerous behavior. Anita uses a wheelchair because she has multiple sclerosis. Today she is distraught. Last night, she forbade Vic to leave the house, but he went anyway. He didn’t come home last night or go to school this morning. Anita has called everyone she can think of, but no one knows where he is. The police won’t help until he has been missing at least 24 hours. Anita has come to you as a last resort. When you saw Vic, you were troubled by his history of uncontrolled behavior and his uncooperative stance. You were hoping to get him to open up in a follow-up visit. But now Anita is here alone, frantic because she doesn’t know where Vic is. What do you do?

Promoting healthy grief
COVID-19 has changed the way children experience the death of a loved one. Although difficult under any circumstance, bereavement is even harder when mourners can’t gather. Barriers to comforting mourning rituals and supportive social communities can make it harder for children to grieve in healthy ways, while increasing the risk for maladaptive grief reactions.

Building family resilience
“Families provide a kind of protective membrane for children when crazy things are happening around them,” said William Saltzman, PhD. Dr. Saltzman is a faculty member of the REACH program Child/Adolescent Training in Evidence-Based Psychotherapies. “Families really have been on the front line throughout the pandemic,” Dr. Saltzman said. “It’s been a rollercoaster ride from the beginning, with abrupt school shutdowns; the exhaustion of becoming the 24/7 caregiver, teacher, playmate, and breadwinner; and now having to figure out largely on their own how to navigate the upcoming school year.”
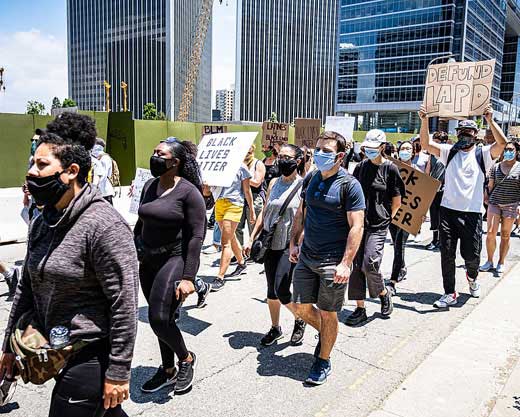
How to talk with patients about racism
Once pediatric primary care providers (PCPs) recognize the importance of having conversations about race with their patients and families, the next question is how to begin.

Your patients need you to talk about race
“The first thing clinicians need to know about racism and discrimination is how important it is to talk about it.” Open, honest, and effective conversations about race and racism are crucial to young people’s mental health.

Helping patients deal with trauma
A medical appointment can be intimidating and scary for a child with a history of trauma. Still, this visit might be the first time a patient shares that they have been sexually or physically abused or that they are terrified to live with their fighting parents during COVID-19. Your role as a primary care provider (PCP) is critical. Your interactions with your patient need to feel safe. As constrained as your time is, you must make every minute count toward establishing a connection.

Alleviating coronavirus anxiety
We don’t have to tell you that virtually everyone feels anxious about the spread of COVID-19. An appropriate level of anxiety can be helpful if it inspires people to follow CDC recommendations on hygiene and social distancing. An unnecessary level of anxiety, however, can impair both mental and physical health. Many of your patients and families are suffering from unhealthy anxiety–whether they present with possible COVID-19 symptoms or come in for an unrelated complaint.
Find the Right Training for You
Browse evidence-based training for primary care clinicians, mental health clinicians, school support staff, and healthcare organizations across the U.S.
BROWSE COURSESBetter Mental Health Care Starts Here.
Get the latest research, training updates, and practical tools
delivered to your inbox. Join thousands of clinicians working to
improve pediatric mental health outcomes.
e-mail address
SIGN UPLATEST
LinkedIn Article 1
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Suspendisse varius enim in eros elementum tristique…
LinkedIn Article 1
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Suspendisse varius enim in eros elementum tristique…
LinkedIn Article 1
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Suspendisse varius enim in eros elementum tristique…
GET IN TOUCH
Name*
Name Surname
E-mail Addres*
name@mail.com
Organization
Your organization
Your Message*
Your message…
